Health Focus – Cushing’s Disease (Hyperadrenocorticism) in pets
CUSHING’S DISEASE
WHAT ARE THE SYMPTOMS OF CUSHING’S DISEASE?
WHICH ANIMALS ARE PRONE TO CUSHING’S DISEASE?
WHAT IS CUSHING’S DISEASE?
Cushing’s disease, also known as hyperadrenocorticism or HAC is a disease in which the body produces too much cortisone. Cortisone is produced by the body in small amounts every day, and functions as a natural anti inflammatory within the body. Cortisone is produced by the adrenal gland, the same gland that produces adrenalin. The adrenal glands lie just in front of the kidneys inside the dog’s body. In some cases of Cushing’s disease (HAC) the part of the adrenal gland that produces the cortisone develops a growth.
This growth can be malignant (cancerous), but is most often benign (it won’t spread round the body like a cancer). Normally the body controls how much cortisone is being produced – the gland will only produce cortisone if the brain produces a chemical known as ACTH and the brain will only produce ACTH if there is too little cortisone in the body. If a growth develops on the adrenal gland, this growth continues to make more and more cortisone as the cells have mutated and do not need ACTH to make them work anymore. A second form of Cushing’s disease comes from the brain itself, where a growth occurs in the pituitary gland that makes ACTH. These mutated cells in the growth continue to produce high levels of ACTH, regardless of how high the levels of cortisone are in the blood, and this ACTH makes the adrenal glands produce tons of cortisone in response.
HAC occurs mostly in dogs and very rarely in cats and the pituitary form is more common in dogs.
WHAT ARE THE SYMPTOMS OF CUSHING’S DISEASE (HAC)?
Although cortisone in small amounts is really beneficial for the body, too much cortisone is really unhealthy. Dogs with Cushing’s disease show exactly the same changes as dogs that are on cortisone tablets daily or get the “itch injection” a little too often. These are the side effects of too much cortisone and the symptoms of Cushing’s Disease (HAC):
- Weight gain – dogs are starving all the time – they even break into rubbish bins to get food after regular meals. Even if their owners put them on diet, they continue to gain weight despite being on diet
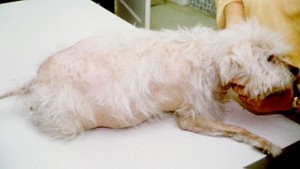
- Weight redistribution – the body moves all the fat onto the belly and chest and dogs develop these huge bellies and fat bodies and little thin legs because the body moves all fat away from the legs.
- Thin skin – if you turn your dog over, you will notice the skin is very thin on his belly and the veins are easily visible
4. Muscle wasting – the muscles of the legs become weaker and thinner and then dogs struggle to get up and down.
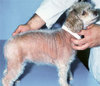
5. Hair loss – the belly is usually bald and the hair loss creeps up round the body, so these dogs have very patchy thin fur generally. Sometimes the fur changes entirely, especially in short haired breeds like the Dachshund
6. Skin infections – the dogs become prone to bacterial skin infections, which itch as well. Often people mistake these for allergies and give the dog more cortisone! If there are pimples in the skin or raised circular areas of skin, it’s probably an infection and not an allergy! Fungal infections like ringworm also become more common, as does Demodectic mange that cannot be controlled with dipping.
7. Dogs are extremely thirsty – they drink bowls of water at a time.
8. Dogs urinate excessively – the urine is very watery (dilute) and dogs cannot control their bladders overnight, often having nighttime accidents. Big pools of urine are produced.
9. Uncontrolled Diabetes mellitis – despite your vet increasing the insulin in your cat or dog that has “suddenly become diabetic”, the blood sugar remains very high. This is very common in cats
10. Dogs are more prone to picking up any infections, especially bladder infections. Cortisone suppresses the body’s immune system, so the body can’t fight disease. This, combined with very weak urine, makes them more prone to bladder infections.
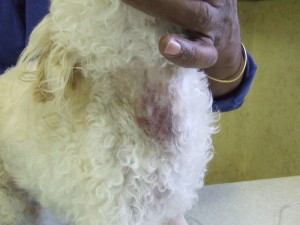
11. Calcium deposits in the skin – these may be very itchy and bright white and hard to the touch. They are usually seen on the belly underneath. Dogs may also get blackheads.
12. Constant panting
13. Darkened skin which bruises easily.
WHICH ANIMALS ARE PRONE TO HYPERADRENOCORTICISM (CUSHING’S DISEASE)?
Dogs get the disease far more often than cats and dogs are mostly small breed dogs, with female dogs being slightly more likely to pick it up. Dogs also tend to be over five years of age when diagnosed.
DIAGNOSING CUSHING’S DISEASE
Cushing’s Disease is diagnosed by either a blood test, urine test, ultrasound or MRI scan. Your vet may recommend a test for Cushing’s disease based on how your animal looks and behaves, especially if he shows many of the symptoms of Cushing’s disease. be aware that dogs on oral or injectable cortisone show the same symptoms and if your dog is on those, you will be wasting your money doing the test. If you are still concerned that your dog has the disease and is also on cortisone, reduce the dose of cortisone gradually and stop it for a month or more. If the symptoms don’t go away, then do the test. Not all the tests are diagnostic on their own, some only say that the test shows that the chances of your dog being positive for the disease are great, but to confirm the disease, you may have to do another test.
Tests for Hyperadrenocorticism:
THE ACTH STIMULATION TEST
The AC TH stimulation test is a blood test for HAC. Your pet will have to stay at the vet for a few hours. A blood sample is taken to measure cortisone levels in the blood, then an injection of ACTH is given. ACTH is the chemical produced by the brain that stimulates the adrenal gland to produce cortisone. A second blood sample is collected approximately 2 hours later.
The test compares the cortisone levels of the first and second samples. If an animal has Cushing’s Disease, the adrenal gland will respond by producing huge amounts of cortisone, way past normal levels. Depending on how much is produced, an animal can be positively diagnosed to have Hyperadrenocorticism if high levels are made, and ruled out from having the disease if the levels only increase slightly. There is a gray area between the two readings, which is non diagnostic and may necessitate your animal having another test to confirm the illness.
THE DEXAMETHASONE SUPPRESSION TEST
This is also a blood test for Cushing’s Disease. Your pet will have to stay at the vet for the day for this test as well. A blood sample is taken to test cortisone levels and then cortisone in the form of dexamethasone is given as an injection to your dog. Up to two more samples are collected over time to check cortisone levels in the blood. A normal dog will respond to the injection by stopping the production of ACTH and thus cortisone, so the levels in the blood would drop. A dog with HAC will not stop or slow down cortisone production and the levels would stay the same or only drop slightly. This test can be used to diagnose Cushing’s disease and also helps to tell the difference between pituitary (brain growth) HAC and adrenal HAC by using low and high doses of Dexamathasone.
THE URINE CORTISOL:CREATININE RATIO
This is a test done on your dog’s urine, so he doesn’t have to stay the day – you can bring in a sample , or your vet can take the sample at his/her rooms. The laboratory measures how much cortisone is in your dog’s urine and relates it to how much creatinine ( a normal chemical found in everyday urine) is in the urine. A ratio is made between the two. In most cases, this ratio will either give you a negative diagnosis (in other words, rule out Cushings disease) or say that the urine strongly suggests HAC and to do a blood test to confirm the disease. In a few cases, the cortisone in the urine will be so high that a positive diagnosis can be made on the urine alone.
ULTRASOUND AND MRI SCANS
Ultrasound and MRI scans look directly at the sizes of the glands inside the body. Both types of scans can assess adrenal gland size, but only the MRI scan can check pituitary gland size. If one adrenal gland is very large and the other is very small, it points to Cushing’s being cause by an adrenal tumor, whereas if both are very large, it points more to the problem originating in the brain itself. The ultrasonographer can also check for any signs of spread of cancer from the adrenal gland if the tumor appears to be malignant at the same time and look for other signs of HAC such as the presence of lots of fat in the liver and abdomen. If the glands are of a certain size, this can be said to be diagnostic for Hyperadrenocorticism.
BLOOD COUNTS AND SERUM CHEMISTRY
Dogs with Cushing’s disease will often have raised liver enzymes (ALT/ALP), especially ALP, also known as Alkaline Phosphatase, due to fat being deposited into the liver. The cholesterol levels in the blood may be elevated, the thyroid levels may be slightly depressed. The white cell count may be increased , especially the neutrophils. Blood sugar may be slightly higher than normal to extremely high in cases with concurrent Diabetes mellitis.
TREATMENT
Medical:
LYSODREN (MITOTANE)
Lysodren is an adrenocorticolytic drug. What this means is that it causes the adrenal cortex (which is the part where the cortisone producing growth is) to lyse or dissolve. This drug has to be given carefully as the body needs cortisone to survive. If too much drug is given, it can dissolve the adrenal cortex entirely and your dog may die at worst, or have to stay on cortisone supplements for the rest of his/her life at best. The dog is put onto Lysodren daily, after being weighed carefully and the exact dose worked out. Because of the dangers of this drug, your dog must have a definitive positive diagnosis of HAC before it can be prescribed, the owner should come into the rooms when the vet is present to collect the medication, have their pet weighed and all the potential side effects of the medication discussed with them. I usually put the dog on Lysodren for 8 days. The owner is instructed to monitor the dog’s appetite and water consumption.
If the dog suddenly stops eating and drinking or looks very lethargic, they are to discontinue the medication and dose Prednisolone tablets (cortisone) as an antidote to their dog and bring it in as soon as possible. If there is a mild decrease in appetite and water consumption, they must keep in contact daily with the vet to assess if they must go on on stop the medication. As soon as the medication is stopped or the 8 days are up, the blood test is repeated (usually the ACTH stim) and if the disease is under control, the dogs are put onto a once weekly dosage of Lysodren for the rest of their lives.
TRILOSTANE (VETORYL, MODRENAL)
This drug works by stopping the production of cortisone in the body, as opposed to Lysodren, which kills the tissue that makes the cortisone. The safety margins are better than Lysodren, but the costs are significantly higher in some countries.
KETOCONAZOLE
Ketoconazole is an antifungal drug which also suppresses cortisone production. It has to be given daily, and is a lot safer than Lysodren, but not all patients respond to it and the costs can also be very high. Dogs that don’t respond well to Lysodren can consider this as an alternative.
ANIPRYL
Anipryl is a new psychotropic drug that was first developed to treat senile dogs. It reduces ACTH being produced by increasing Dopamine (brain chemical) levels. 40-80% of dogs respond well to this drug, but its use is controversial and it is not licensed in many countries. It is expensive and takes 1-3 months before it starts to work. It is only used to treat Pituitary dependent HAC.
RADIATION THERAPY
In some countries, radiation of the Pituitary gland in Pituitary dependent HAC is performed. If the growth in the Pituitary gland is so big that it is putting pressure on other parts of the brain and for example, causing blindness, then these dogs can be irradiated to shrink the growth initially before putting them onto drugs to stop the production of cortisone. It is expensive and the dogs need a general anesthetic every time, so it may not be advisable in very old dogs.
Surgical:
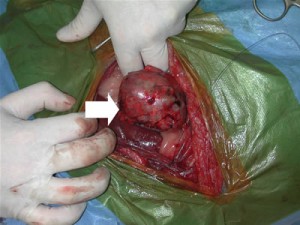
In Cushing’s Disease that is caused by a tumour in the adrenal gland, the whole gland can be removed. This is specialist surgery as the animals may go into shock after the surgery and will require hospitalization to stabilize them afterward. There is no point in removing a gland that has a malignant cancerous growth in it, so the nature of the growth should be checked by needle aspirate and full ultrasound and/or X rays of the chest to check for metastasis before surgical removal. In some countries, such as the Netherlands, the pituitary growth can also be removed surgically.
REFERENCES:
1. http://www.kateconnick.com/library/cushingsdisease.html
2. http://www.pets.ca/encyclopedia/cushings_dog.htm
3. http://www.wellsphere.com/wellpage/cushing-disease-in-dogs
4. http://www.vetinfo.com/dpcush.html
5. http://www.michvet.com/library/medicine_cushings.asp
6. http://www.goldbamboo.com/pictures-t8429.html




Leave a Reply
You must be logged in to post a comment.